Affordable Care Act Enrollment in New Hampshire 2026: What Happened, What It Means, and What Comes Next
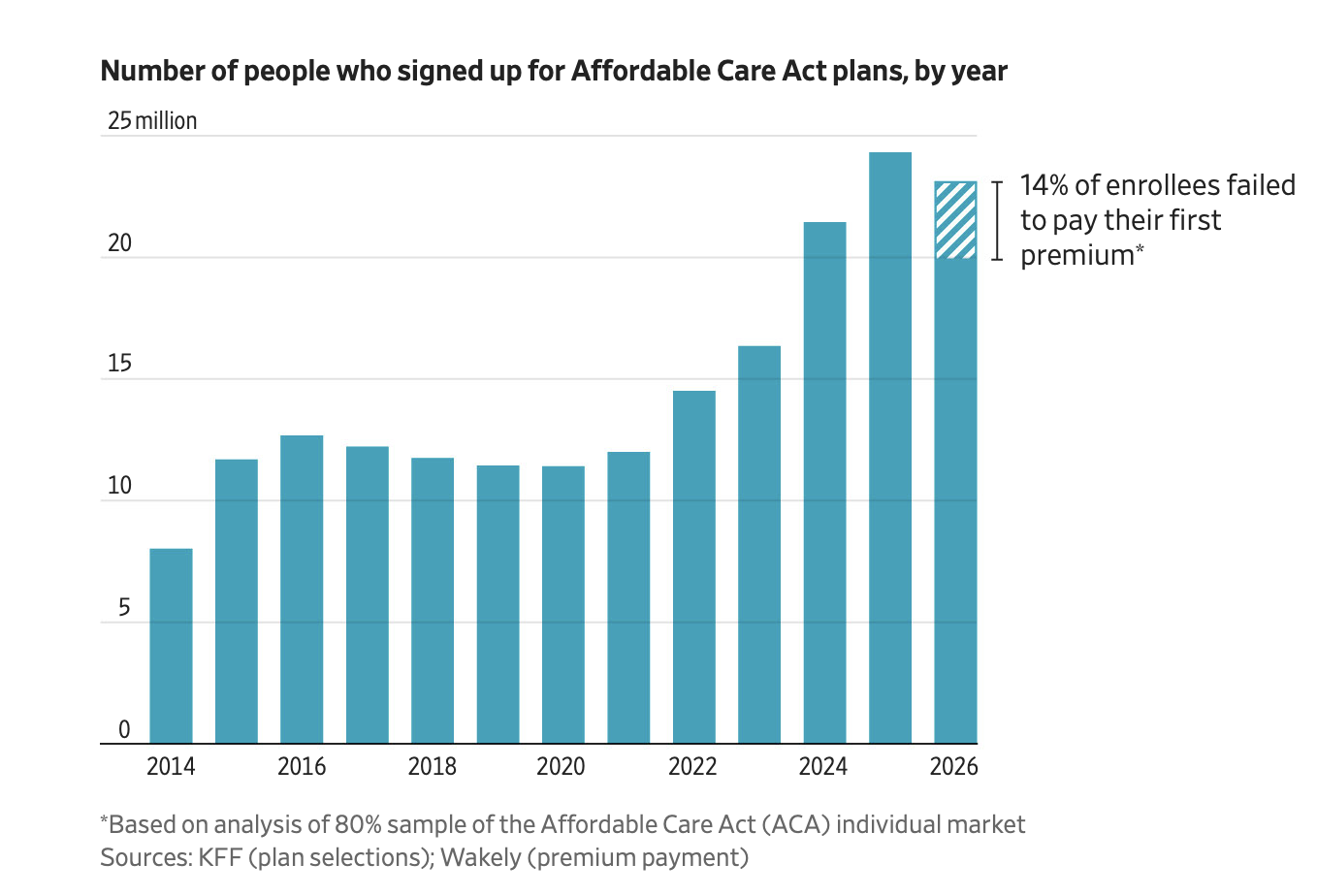
Source: Wall Street Journal
New national data are beginning to clarify just how significant this year’s changes have been in health insurance coverage. Following the loss of federal tax credits that had helped make coverage affordable for millions of families, more than one million Americans dropped coverage entirely.
When early results were first released back in February, enrollment declines were widespread, with 41 states reporting lower figures in 2026 than 2025.
New Hampshire experienced an initial decline of 6.1 percent, down from 70,337 enrollees to 66,024, with more than 4,200 Granite Staters dropping from the program from year to year. And that was only the beginning of the decline.
In the two months since that early report, one in seven Americans who initially enrolled in Affordable Care Act (ACA) coverage for 2026 have not paid their premiums. That’s an additional 14% drop, a loss of another 3 million enrollees. Analysts estimate that overall ACA enrollment is headed for a decline of 17% to 26% before the end of the year.
Against that backdrop, New Hampshire’s latest enrollment experience tells a story that is both concerning—and, in some ways, more stable than what is unfolding nationally.
After reaching a record high in 2025, enrollment through the ACA marketplace declined this year. A clearer picture of enrollment changes will emerge later this summer, when more comprehensive state-by-state data are typically released. And, if New Hampshire’s experience follows national trends, and one in seven drops coverage, then we may see nearly 10,000 additional enrollees lose coverage.
While any decline is concerning, New Hampshire’s experience mirrors national trends—and, on some measures, the state has fared better than others. In other ways, we may have missed opportunities to retain coverage for more people. Understanding more about why enrollment fell, and what that means going forward, is essential for both public health and household financial stability.
A Step Backwards After Historic Gains
The latest decline comes after several years of steady growth in ACA enrollment. Enhanced federal premium tax credits, expanded outreach, and rising awareness pushed New Hampshire’s insured rate to a record high in 2025.
Those gains were built over more than a decade and will not disappear overnight—but 2026 represents a turning point toward a worrisome enrollment decline.
As premiums rose sharply leading into 2026, outreach efforts like patient navigators and enrollment counselors were mostly eliminated. New Hampshire, which relies on the federal marketplace, felt these pressures directly. For residents who purchase their own health insurance, the ACA remains one of the most important pathways to coverage. But this year’s enrollment season came with a harder reality: coverage is still available, yet for many people it now costs significantly more; and for thousands of others, coverage is financially out of reach altogether.
What Comes Next
For New Hampshire, much will depend on future policy decisions, affordability trends, and whether additional steps are taken to stabilize coverage and provide consumer assistance. A deeper look into the factors driving affordability, access and enrollment is important to inform next steps.
Program Cuts from Washington and Inaction at Home
Several forces converged during the enrollment cycle that should be noted. These trends help explain what we are now seeing in both national and state-level data.
Federal subsidy uncertainty. Congress failed to permanently extend the enhanced ACA tax credits that had made coverage affordable for tens of thousands of New Hampshire residents since 2021. As a result, insurers priced 2026 plans assuming those subsidies would expire, contributing to higher premiums.
Mariana Poore served as Coordinator of Health Insurance Navigation at the Foundation for Healthy Communities during the latest enrollment cycle. She stated these financial pressures landed unevenly on consumers. “With the expiration of premium tax credits, some people faced dramatic shifts,” she noted. “One young woman I worked with went from paying $20 a month last year to $101 this year on the same income.”
Premium pressure. Insurers across the Northeast imposed significant rate increases, driven by hospital consolidation, rising pharmaceutical costs, workforce shortages, and higher utilization post-pandemic. For many families, sticker shock alone was enough to abandon enrollment.
“People were questioning whether they could afford to stay in the marketplace at all,” Poore shared. “Families moved from gold plans to bronze plans just to keep something, and we don’t know how many will continue to afford the plans they signed up for throughout the year.”
The highest premium increases for 2026 were faced by older adults (age 50-64). More than 50% of all enrollees who lost eligibility for tax subsidies were in this age bracket. Many older enrollees were already in the lowest-cost bronze plans and had no cheaper options to step down to.
Navigator/Consumer Assistance cuts. At the same time that subsidies expired, the federal government slashed funding for ACA Navigators by nearly 90 percent. In New Hampshire, that meant the loss of most local, in-person enrollment assistance—these cuts were especially damaging in rural areas and for residents with limited internet access or language barriers.
“We had hired a team of six navigators for the cycle. Then we found out that 92% of our funding had been cut, and went from six navigators to one,” recalled Poore. “The remaining 8% was directed to the call center, and I had to recertify as an application counselor to keep supporting people.”
State Inaction. Unlike some states that stepped in with bridge funding, supplemental outreach, or state-based affordability programs, New Hampshire offered no new state resources and pretty much directed consumers to rely on community organizations to fill the gaps. Without state investment in consumer assistance or patient navigators to meet the need, the downsized program that Poore coordinated had limited reach. Moreover, that program has now expired altogether and is no longer available to consumers in need of future enrollment support.
What Other States Did to Maintain Affordability and Protect Coverage
Several states adopted state-level strategies that helped cushion the blow for their residents. These investments and policy interventions include:
State-Based Marketplace Subsidies and Special Enrollment Periods
States that operate their own ACA marketplaces—known as State-Based Marketplaces (SBMs)—had more flexibility to tailor enrollment outreach, extend deadlines, and design targeted plans for their residents.
Some moved proactively to mitigate the impact of federal subsidy cuts. Connecticut launched a special enrollment period with new state subsidies targeting households affected by the loss of enhanced federal tax credits. Backed by roughly $70 million in state funds, the initiative allows eligible residents to receive state-supported premium credits that partially replace the lost federal assistance and stabilize premiums. Other examples include California’s Covered California and Colorado’s marketplace - states that were monitoring enrollment trends in real time rather than relying solely on the federal platform.
In total, 10 states and the District of Columbia offered state-based premium assistance or cost-sharing reductions, to supplement or replace the federal tax credits that expired at the end of 2025. These initiatives were aimed at preventing massive premium hikes for residents in state-run marketplaces. Even modest state-level investments and strategies in SBM states have helped retain people with coverage during policy uncertainty.
Expanded Outreach and Extended Deadlines
In Pennsylvania, community health advocates and state insurance officials worked together to extend the open enrollment deadline and to highlight enrollment through events and local forums—an example of how state agency outreach campaigns and partnerships with advocacy organizations can support enrollment despite federal challenges.
Who Is Most Likely to Lose Coverage?
Low- and moderate-income individuals were most likely to drop health insurance as costs rise, and particularly younger adults ages 19–44. The end of pandemic-era Medicaid continuous enrollment has already pushed millions off Medicaid and is expected to continue affecting ACA coverage rates.
Younger adults, healthier individuals without ongoing medical needs, and people seeking lower-cost or catastrophic plans are more likely to opt out when affordability declines. Coverage losses also disproportionately affect communities of color, including Latino adults, who already face higher uninsured rates.
The disability community is among the most vulnerable to coverage instability. Lisa Beaudoin, Principal Consultant of Strategies for Disability Equity, described how families have been affected:
“The paperwork burden on caregivers is enormous, meaning that people with disabilities can end up uncovered for weeks or months at a time. Losing coverage even briefly can threaten their health and continuity of care,” Beaudion shared. This is true for both Medicaid and the Health Insurance Marketplace.
Where New Hampshire Did Better Than Many States
Despite these challenges, New Hampshire’s ACA enrollment had some notable results:
The state still maintains one of the lowest uninsured rates in the country,
Most residents who lost coverage did so due to cost and complexity, not eligibility,
The marketplace itself remained stable, with insurer participation intact.
These are signs of a system under strain. Many recent studies show that access and affordability are still real barriers even for those with insurance. Co-pays and high deductibles mean that even those with insurance struggle to pay for care in New Hampshire - basically, health insurance is not enough to feel health security anymore.
Where We Go From Here
The takeaway for 2026 is fairly stark: the ACA is still essential, but it has become harder for many people to benefit as intended. The law continues to provide a critical pathway to coverage, especially for people who do not get insurance through an employer. But with enhanced subsidies gone, the Marketplace is expecting that individuals and families will absorb much more of the cost themselves. That means enrollment assistance matters even more as costs soar, and plan selection can make the difference between staying covered and going uninsured. In other words, the ACA remains a lifeline in 2026, but for many households it is now a more expensive and more fragile one.
New Hampshire entered 2026 from a position of relative strength—but will need state policy attention to achieve resilience in the Marketplace.
The early decline in enrollment reflects real pressures on families navigating rising costs, fewer supports, and growing uncertainty. If those pressures continue unaddressed, January’s drop in coverage will hit double-digits in the Granite State before the end of the year. The 2026 enrollment numbers should be read as a warning, but not a final verdict.
There are clear paths forward:
Restoring navigator funding—or replacing it with state funding sources—would help ensure access is informed, equitable, and not dependent on ZIP code or digital literacy.
State leadership and investment could play a stronger role in outreach, education, and consumer protection as costs continue to rise.
Federal action to renew enhanced premium tax credits would immediately improve affordability.
Most importantly, coverage must be treated as what it is: a foundation for economic stability, workforce participation, and community health.
“The negative downstream effects of losing coverage cost far more than maintaining it,” Beaudoin warned.
Health Insurance enrollment through the Affordable Care Act remains one of the most powerful public health tools we have. Protecting it—and the people who rely on it—will require action, coordination, and renewed political will in the year ahead.